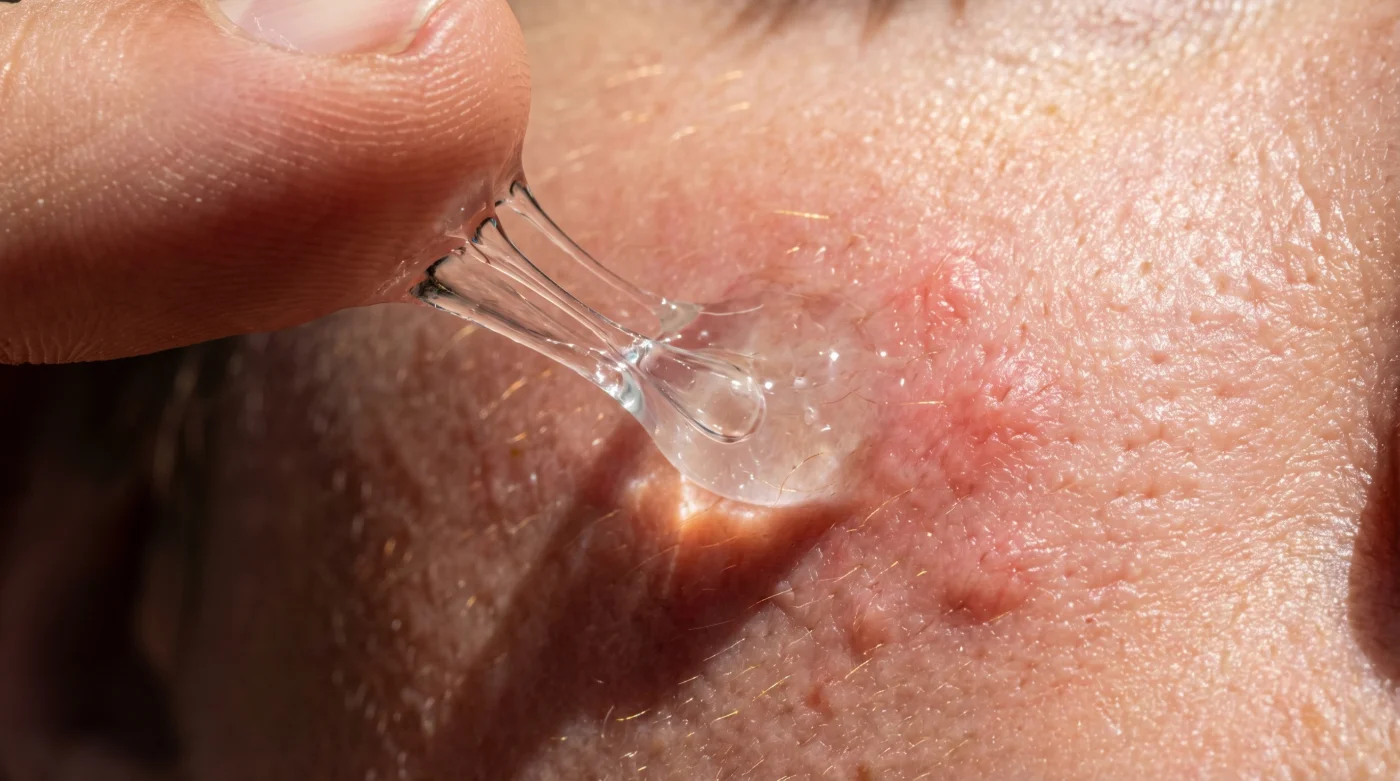
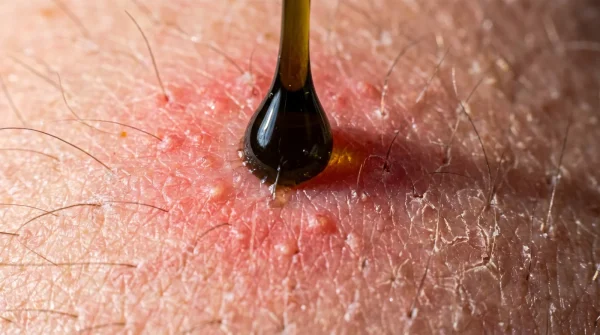
The glass dropper dispenses a thick, translucent ribbon of serum. It pools on your fingertips, cold and slightly stringy, carrying the faint, clinical scent of a sterile lab. You press it into your cheeks expecting the glass-skin hydration promised by countless internet routines. Instead, within twenty minutes, a tight, creeping heat radiates from your jawline. The skin does not just flush; it erupts in tiny, angry clusters of micro-welts. You are experiencing pan-allergy cross-reactivity. At a molecular level, the proteins in snail mucin share nearly identical structures with house dust mites. Your immune system cannot tell the difference between this viral sensation and the microscopic pests living in your mattress.
The False Promise of Universal Hydration
Think of your immune system like an exhausted bouncer at a crowded nightclub. It operates on a strict list. When you apply this secretion, the bouncer checks the protein signature. Because the glycoprotein structures in the formula are so biologically similar to dust mite excrement, the bouncer panics and sounds the alarm.
The beauty industry markets this sticky substance as a universally tolerable healing agent, a miraculous soothe-all for a compromised skin barrier. But if you sneeze when sweeping the attic, applying this serum is the immunological equivalent of rubbing a dust bunny directly into your pores. The resulting histamine cascade is not a simple breakout; it is an active rejection, demanding immediate intervention rather than another layer of moisturizer.
Recalibrating the Barrier Response
When the inflammatory flush hits, you need to act with clinical precision, not panic. You must immediately interrupt the histamine cycle. Strip the surface completely with cold water and a basic glycerin cleanser before moving on to the next steps.
- Constrict Capillaries: Wash the area with ice-cold water. You want the water cold enough to physically shrink the blood vessels, visibly slowing the red flush from spreading across your cheeks.
- Neutralize the Reaction: Apply an over-the-counter 1% hydrocortisone cream to the affected zones. Watch for the skin to shift from a bright, angry red to a dull pink within thirty minutes.
- The Antihistamine Intervention: Dr. Aris MacMillan, a clinical immunodermatologist, relies on a simple internal defense. She advises taking a second-generation oral antihistamine like cetirizine immediately upon seeing the micro-welts. Treat it like a bee sting, not a bad lotion, she notes.
- Skip the Occlusives: Avoid sealing the reaction under heavy ceramide creams or petroleum jelly. Trapping the heat will only amplify the swelling and leave the skin feeling suffocated.
- Cold Compress Protocol: Wrap ice in a clean cotton t-shirt and press it firmly against the jawline. The tactile cue here is numbness; once the skin feels dull to the touch, remove the ice to prevent thermal damage.
- Identify the Baseline: Wait a full 48 hours before introducing any active ingredients back onto your face. Your barrier is highly reactive right now and needs complete rest to stabilize.
Managing the Histamine Fallout
The immediate aftermath of a mucin reaction leaves the skin unpredictable. People often mistake the tiny, fluid-filled bumps for a sudden acne purge and attack them with salicylic acid. This strips an already damaged barrier and turns a temporary allergic flush into weeks of flaking dermatitis.
You need to read the signals correctly. For the purist, stick exclusively to a single-ingredient hypochlorous acid spray for three days. It kills surface bacteria without triggering any immune response. If you are in a rush, tap a colloidal oatmeal liquid directly onto the worst patches before leaving the house. It leaves a slight matte film but physically binds to the skin to block environmental irritants.
| The Common Mistake | The Pro Adjustment | The Result |
|---|---|---|
| Using salicylic acid on the bumps | Applying 1% hydrocortisone cream | Reduces swelling without stripping lipids |
| Slugging with petroleum jelly | Leaving the skin open and dry | Prevents trapped heat and redness |
| Testing a new soothing serum | Reverting to hypochlorous acid | Stabilizes the immune barrier safely |
The Reality of Biological Skincare
We have grown dangerously comfortable treating biological secretions as casual cosmetics. Understanding the molecular overlap between what heals us and what harms us forces a necessary shift in how we approach consumption.
Your skin is not a blank canvas waiting to be painted with the latest viral export; it is a highly intelligent, reactionary organ. Learning to anticipate its boundaries, rather than forcing it to tolerate biological triggers, strips away the anxiety of the daily routine. You stop fighting your biology and finally start working alongside it, achieving a calm, predictable complexion based on science.
Frequently Asked Questions
Can I build a tolerance to snail mucin over time? No, continuous exposure to an allergen typically worsens the reaction. Your immune system will only mount a faster and more aggressive defense with each application.
Are vegan snail mucin alternatives safe for dust allergies? Yes, because vegan alternatives rely on plant-derived glycoproteins like wild yam root. They mimic the texture and hydration without carrying the problematic animal proteins.
How long does the cross-reactive breakout last? The acute redness usually subsides within 24 hours with proper antihistamine treatment. However, the textural bumps may take up to a week to fully flatten as the skin cycles.
Is this reaction limited only to my face? The reaction is localized to wherever the protein touches the skin, but severe allergies can cause systemic itching. Always wash your hands thoroughly after accidentally touching a reactive product.
Will a patch test prevent this kind of severe breakout? A patch test on the inner arm is highly effective for identifying this specific cross-reactivity. The skin there is thin enough to show an immune response before you risk your entire face.